Stem Cells and Neurodegenerative Diseases: The Search for an ALS Cure
- Rowan Blade
- Oct 24, 2022
- 3 min read
Scientific research is a prolonged process riddled with failure and roadblocks. In recent years, there have been numerous failed clinical trials that hoped to cure neurodegenerative diseases like Alzheimer's disease, despite the leading theory having 15 years of funded research supporting it.
With the prevalence of failure, how can there be hope in the study of neurodegenerative diseases? One of the main reasons why most of the research on neurodegenerative diseases has failed is because scientists still do not understand the reasons why the body fails to correct damage to neurons. This lack of understanding of the mechanisms behind the disease is partially responsible for the difficulty in studying deadly diseases that likely have multiple causes, like the disease ALS, amyotrophic lateral sclerosis.
ALS is a progressive neurodegenerative disease that has historically been associated with damage to motor neurons, causing motor deficits like leg weakness and uncontrollable movement. Most often, patients die within 2-5 years from respiratory failure caused by those motor deficits. Scientists know little about the disease's direct cause and inner workings, which limits the effectiveness of medications that try to slow the progression of the disease and protect the damaged neurons. About 10% of the disease is caused by heritable mutations in genetic code, but 90% of ALS cases do not have a known family history, or are sporadic.
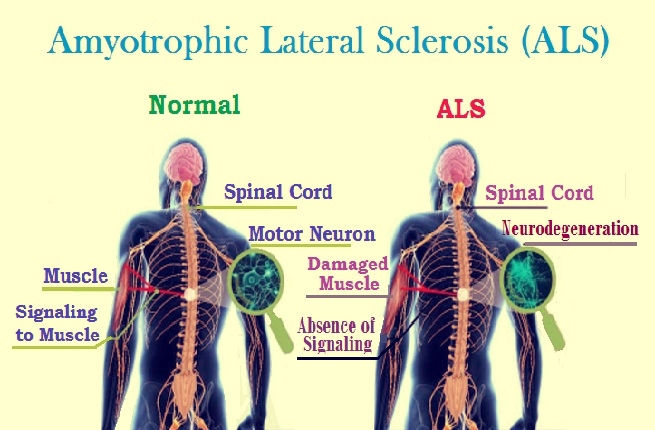
Visual depicting the effect of ALS. Source: Scientific World Info
The FDA has approved two medications for the treatment of ALS. Riluzole is a medication that acts as a neuroprotector by preventing the release of glutamic acid, which is thought to injure neurons and contribute to ALS pathology. It is often the first medication prescribed and though there have been variable accounts of the long-term success rate, one study found that the drug significantly increased the 1-year survival rate of patients who received treatment.
Another medication, Edaravone, may trap free radicals in the body that contribute to neuronal stress, which is associated with motor deficits in ALS patients. Initial studies believed the treatment would have greater effectiveness in patients who began treatment with greater motor control, but a 2022 study indicated that there was not a significant long-term benefit to the treatment.
One way to measure the disease progression in patients is the ALSFRS-R scale, which measures ALS symptoms from the disease’s onset and through treatment. There are 12 categories used to measure function, such as breathing ability, speech, swallowing, and walking. Patients rate their ability to complete these daily tasks on a scale from 0-4 and disease progress is measured by the decrease in points over time. Many studies also use direct limb weakness as a measure of disease progression.
In a 2021 study, researchers injected mesenchymal stem cells (stem cells found in bone marrow and primarily used for the repair of bone) and neurotrophic factors (which support the survival and growth of neurons) into participants in the hope of slowing the disease progression as measured by the ALSFRS-R scale. The study used the levels of several biomolecules as internal indications of disease progression in patients, some of which measured neuroprotective ability, inflammation of the neurons, and neuronal damage. Though the study did not find any significant change in the loss of function of the participants, the markers used to monitor neuronal degradation and inflammation decreased with the treatment. Though this does not directly lead to a cure or a new treatment, it may open more opportunities for research into the cause of neurodegeneration.
In a 2022 study, researchers injected astrocytes (a type of cell that protects diseased neurons) into one side of a patient’s spinal column to target the protective astrocytes to one of the patient's legs. The other leg was left as a control in order to monitor the effects of the drug on each patient without the variability common in most neurological studies. The presence of the introduction of healthy astrocytes was believed to be able to slow the damage of motor neuron disease, but this clinical trial also did not prove to be statistically significant in slowing the rate of disease progression. However, all of the grafts of astrocytes in the study survived, and the delivery method was proven to be relatively safe. This also does not directly lead to a cure, but an effective delivery method with reliable control will help clinical trials in the future to have more accurate results.
Despite the best efforts of the scientific community, there is not yet a cure for ALS and many other neurodegenerative diseases. Many recent scientific studies are searching for the cause of sporadic ALS and how the disease changes the people affected by it, both in physical function and in internal biological processes. Hopefully, gaining an understanding of the actual changes ALS makes on the body will help to target research in clinical studies and find a way to stop or slow the progression of the disease.






Last year, my 68-year-old partner was diagnosed with Lou Gehrig's disease also known as ALS. Speaking and swallowing were two of his challenges. His collapse was swift and catastrophic, and neither the riluzole nor the medical staff did much to aid him. He would not have survived if our primary care physician hadn't given him attentive care and attention, as the hospital center didn't provide any psychological support. His fall was abrupt and catastrophic. His hands and legs gave way to weakness in his arms. This year our family physician suggested using vinehealthcentre. com ALS/MND treatment, which my husband has been receiving for a few months now. I'm delighted to say that the treatment greatly reduced and reversed his symptoms…